DRC: Kinshasa lifts the Mpox-related public health emergency
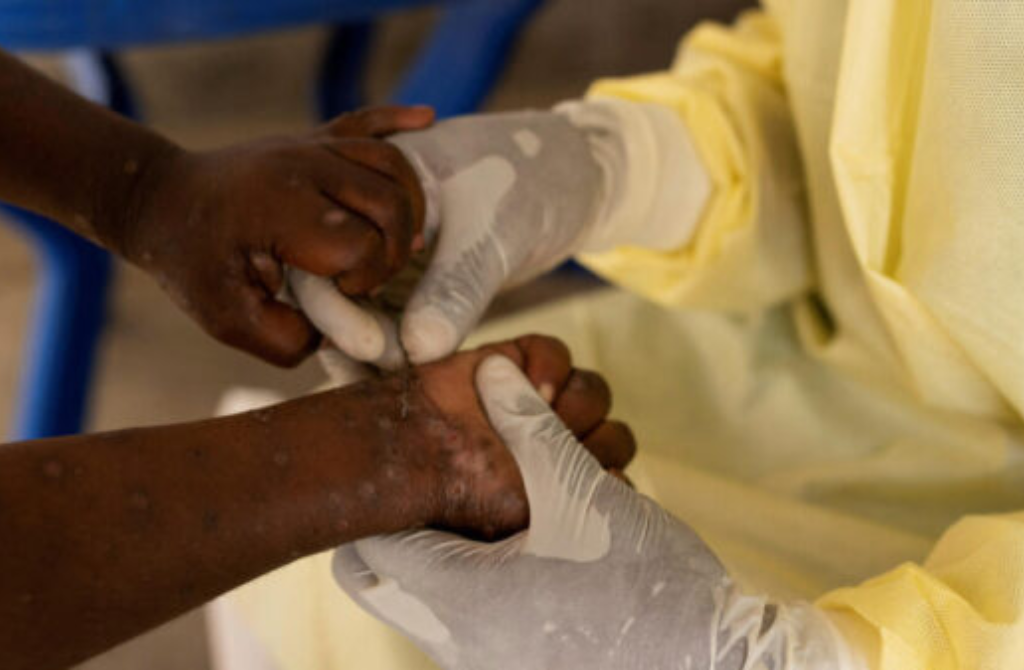
The Democratic Republic of Congo (DRC) is closing a health chapter that has tested both its resilience and its institutions. After more than three years of struggle, the government has declared the end of the Mpox epidemic as a national public health emergency. The announcement, made in Kinshasa by Health Minister Roger Samuel Kamba, comes amid a continental lull, as Africa CDC and the World Health Organization have lifted their alert mechanisms.
At the peak of the crisis, in early 2025, the country recorded nearly 2,400 cases per week. Today, there are around 170. More than 124,000 cases have been recorded since 2022, hitting children hard as well as provinces already weakened by insecurity.
The decline does not erase the memory of logistical tensions, initial vaccine shortages, or regional disparities. Nevertheless, it attests to a methodical recovery.
The strategy claimed by the authorities rests on a deliberate centralization: one plan, one budget, one coordination.
This architecture made it possible to avoid the fragmentation of responses that had sometimes handicapped other crises.
In three years, the country has gone from two to nearly sixty operational laboratories. More than 1.5 million people have been vaccinated. Behind these figures lie a learning administration, trained teams, and shortened decision‑making circuits.
A prolonged epidemic weighs on productivity, disrupts schools, and weakens households. Bringing it under control frees up room for action. It reassures investors, consolidates international credibility, and strengthens the state’s capacity to plan.
The cost of the response, estimated at around $90 million, contrasts with the expenditures incurred during Ebola for a far lower number of cases. This budgetary efficiency marks real progress in health governance.
Nevertheless, the virus still circulates. Vigilance remains necessary, particularly in the east of the country, where insecurity complicates access to care.
Consolidating the gains will require embedding new capacities permanently into the ordinary framework of the health system, beyond the logic of emergency response.
The Congolese experience offers a valuable lesson. It shows that an African state, despite structural constraints, can structure a coherent response, control its costs, and strengthen its institutions.
The end of the epidemic is not a final stop. It is proof that health sovereignty is built through effort, discipline, and steadfastness. It is on this foundation that the next stage of Congolese development will depend.